
Hannah can't get enough of her big brother -- she pulled him in closer for hugs and demanded her "cheek kisses" when she was lying on the floor!
Hannah is definitely on the mend. She only has 2 more days of Cipro left for her trachiitis (pseudomonas), and we are finally starting to see her old personality come back. She is not as exhausted all the time (no more 3-long-nap days), and she is willing to be more engaged and is wanting to be more active. She also had a fantastic therapy session with her Early Intervention specialist today, so I knew my “old Hannah” was coming back to us.
The older kids had their Fall Festival at their school tonight. It ran from 4 pm until 7 pm. It was a big event for the school, and my sister-in-law, nephew, and two nieces were going to come join us.
I was getting kind of hesitant about going around 3:30 pm. Hannah had not taken a second nap yet, which was unusual for her. She usually crashes after her therapy session and sleeps until around 4 pm.
But the kids were so excited to go. I decided that since Hannah had such a great day and was obviously feeling better that I would take a chance with her. So we all piled into the car and headed to the Festival.
She did pretty well in her stroller for the first 20 or 30 minutes or so. Then I could see her exhaustion setting in… the eyes rolling back, the droopy head, and then the crying. That silent cry that always makes me nervous because I fear another breath-holding spell (leading to seizure) again if I don’t pick her up and console her.
From that point on, I had to carry her. She clung on to me but was still awake. After about 20 minutes or so of holding her, my arms and back were starting to hurt. Of course, she took that as a cue to cradle down in my arms and get into her “I’m going to sleep” position. She fell asleep finally, and after about 5 minutes I put her in the stroller.
Of course, she immediately woke up and started crying again. From that point on, she was inconsolable. No matter what position I tried or how I held her, she just would continue crying and thrashing. But the older kids were having such a great time that I felt I had to try everything not to cut the night short and head home.
I thought that maybe if we sat down and let the kids grab a bite that I would be able to get her back to sleep. But go figure, the food area was right next to the loudspeaker and all the noise and activity. Hannah went into sensory overload, and I could not get her to calm down at all.
I had to admit defeat. I told my sister-in-law that I had to take Hannah home. She offered to keep Abby and Ethan with her and take them home later, but the truth was that I needed to have the kids in the car with me to help me try and get home. Hannah does not do well in the car as it is, and I honestly don’t know how I would make it home without having to stop 50 times along the way.
I told the kids we were going to have to go. Ethan and Abby were disappointed. But Ethan accepted it immediately and worked on helping me get the stroller together for the walk back to the car. Abby was a bit more upset. My nephew, who was not used to these “well Hannah is upset so our plans change again” episodes, was so adorable and kept saying “It’s okay Abby. I’ll come to your house and we can play.” Even though Abby was upset, it was very short-lived because she knew that we needed to get Hannah home.
As my sister-in-law and I parted ways in the parking lot of the school, my kids and I were trying to get everything in the car. I tried to get Hannah into her car seat, and she started with her hyperventilating spell and was so horribly upset. I kept thinking to myself “Please, not here. Please, calm down.” It was horrible. As Abigail got into her seat, I took Hannah from her car seat and sat up in the front passenger seat just trying to rock her. I started the car and blasted the cold air on her back because she was sweating and very heated from her agitation.
I didn’t realize how amazing this was at the time, but as soon as I started rocking Hannah in the front seat, Abby came over to us behind the seat and started singing “Twinkle, Twinkle, Little Star” to Hannah (this is our “go to” song when we need to try and calm her down). Then, I heard the back door of my mini-van shut. Ethan had taken it upon himself to empty out the stroller (huge diaper bag, suction machine, etc.), put the stroller in the trunk, and organize Hannah’s bag and suction machine in their respective places we keep them in the car.
About 10 minutes later of sitting in the car, Hannah finally passed out. She had worked herself up so much that she was still trying to catch her breath as she slept, but she was calm and comfortable. I was able to get her into her car seat. As I got into my driver’s seat, I saw Abigail covering Hannah up with a light blanket. She held Hannah’s hand the entire way home.
As we all piled back into our house after our Fall Festival adventure, I put Hannah on the living room floor where she slept for over two hours. The other kids, my sister-in-law, and I shared a quick McDonald’s dinner that my sister-in-law picked up on the way over. Then the other kids went off and played — my nephew and Ethan on the Wii, and Abby and my older niece (almost 2) in my office.
I am so proud of Ethan and Abigail for their sacrifices they make for Hannah. They are so damn good with her. Even though they may initially complain, it never lasts long, and they never blame her. Even my nephew surprised me tonight because he was also having such a good time at the Festival because I thought he would not understand why we had to just “up and leave.” But he did. He was awesome about it.
I know that Hannah has her limitations, and I know that I still have to keep trying to push her a little bit each time so that the older kids can still have their fun and activities. I just feel so lucky that the kids accept that their little sister just can’t handle it all the time and love her unconditionally even if it interrupts our plans.

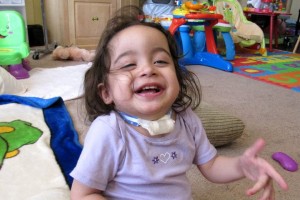 This movement disorder she acquired when she was hospitalized this summer is really doing a number on her. I don’t know if it is her actual choreathetoid movements getting worse or if she is just growing a tolerance to her medications (Keppra, Klonopin, and Haldol).
This movement disorder she acquired when she was hospitalized this summer is really doing a number on her. I don’t know if it is her actual choreathetoid movements getting worse or if she is just growing a tolerance to her medications (Keppra, Klonopin, and Haldol).

Latest Comments