It is only 10:30 am in the morning, and things are really busy around here!
At rounds this morning, there was a new attending that we had never seen before, an older man. I really liked him because he really shook things up with Hannah’s care and got the fellow and residents to think more about Hannah as a patient than as a puzzle that needed figuring out. He also has been the first attending to really get me involved, asked me a lot of questions about her needs, and I really appreciated that.
He immediately wanted to get Hannah set up on a CPAP trial in order to try and get her closer to a humidified trach collar off the vent. There was a controversy about how long to have the trial during rounds between the fellow and the resident, and he said “why don’t we just let her decide how long to do the trial. Don’t set a time limit for the trial or stick to so-many-times per day. If she can go 20 minutes, then do it 3 or 4 times a day. If she can go longer, then we will do less trials a day.” FINALLY, a doctor with logic!
So Hannah is currently on her CPAP trial. One hour so far, and she has done really well.
There is FINALLY concern about her not getting enough calories thanks to this attending. I have brought it up numerous times, but everyone felt that the TPN was good enough coverage. When I said that she used to get between 1200 to 1500 calories a day, and she was basically maintaining her weight. Come to find out that TPN was less than 700 calories a day PLUS she is burning more by moving around constantly…. well, this became a priority conversation. So, it was decided that since her central line has to come out anyway (it has been in for a month now), she is going to get a PICC line tomorrow so they can continue TPN plus be able to work on getting her feeds up (she has been at 10 mL/hour but was having trouble progressing to more because of sedation/movement issues). They are going up 5 mL/hour every 4 hours today up to 30 mL (I believe). Hopefully now that she is off most of the sedation meds (all her IV drips were finally done as of last night), her bowels can start working better.
Physical and occupational therapy came by today to do their assessment. They sat her up to see how her tone was, and it was great to finally see her sitting up after a month laying in bed. She had to be completely held up since her body was still flailing, weak, and she can’t control her neck muscles that well just yet. They have set her up for PT and OT every day, and they gave us some exercises to do with her as often as possible in order to help her muscles since they contract so tightly during these movements.
She has an echocardiogram set up for some time today to rule out a strep infection and/or endocarditis causing these movements (rheumatic fever type of syndrome). They also did a blood draw for ASO titers to check for strep as well.
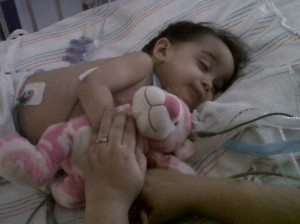
The BEST part is that Hannah now recognizes me and Daddy again. I didn’t want to post about it yesterday in case it was a fluke, but when we sing her favorite songs to her now, she starts smiling really big, and you can hear a little giggle (for some reason, not all her sounds are muffled with the trach). OMG, it was awesome. We had all the nurses come in to see her do it (especially since most of them have had Hannah at some point). We have done it multiple times now, and we even got a video of it.
I see Neurology outside in the hallway at another bedside, as Hannah’s nurse is starting her Cerezyme. I hope they will come in here after and give us more idea of their game plan.

Latest Comments