We had our meeting with the pulmonologist today. I knew from Daddy’s meeting with him 6 weeks or so ago that this doctor was going to be very conservative about the talk of getting rid of the trach. So I came into the appointment with the mindset to just have him understand our point of view on why we want to discuss the possibility of decannulization.
He was a nice enough doctor, older, gray-haired.
I told him about what happened when Hannah pulled out her trach yesterday and how I called his office yesterday and the receptionist said that there were only general pediatric residents available, no one who was really familiar with trachs and what to do when we had to put in a smaller one, etc. The doctor immediately got pissed off and said “Excuse me,” and left the room. Hannah’s nurse and I were sitting in the room thinking “what the heck?” and we heard him reprimanding his nurse because I guess she was not available when I called (I had gotten her voice mail and didn’t leave a message, pressed zero to talk to someone). The nurse came in and apologized profusely and told me in the future to have her paged if this happens again.
Next thing he said was that we should have taken Hannah to the ER immediately if we could not get the right trach size back in and that the hole was probably closed up now around the new 3.0. He doesn’t like keeping Hannah on the 3.0 because it is a smaller cannula, and with the amount of junk she gets at times, it could get clogged. Fair enough.
I brought up the topic of decannulization, and I swear that he changed personality. He was so set in his thought process that Hannah will never be decannulized because of the POSSIBILITY of her Gaucher progression affecting her airway. He made the comment “I already told your husband that it is not something we should consider.” EXCUSE ME? I was completely taken aback by his change in attitude.
The conversation continued like this:
Me: “I really would like to consider the possibility since Hannah was trached not because of airway issues but because she was oversedated when she was intubated.”
Doctor: “Even despite her prognosis, she had airway issues which is why her extubation failed numerous times before she was trached.”
Me: “She did not have any airway issues before she was trached. Again, she was trached because they could not get her off sedation enough to maintain her breathing on her own.”
Doctor: (Blowing me off and ignoring my reiteration) “I have the notes here as to why she needed to be trached. Besides, her tonsils are so big, she would have breathing problems as well with that.”
I looked at Hannah’s nurse who was with us, and she and I just looked at each other like “Are you friggin’ kidding me?” It was obvious that he would not even consider the possibility, so I decided to drop the subject for now.
Because I wanted to get Hannah a passy muir valve (so she could learn to use her voice), I just dropped it for the time being and talked about getting her a passy muir valve (which will hopefully be ordered tomorrow). He also made the comment that he wanted to get Hannah in to see her new ENT sooner than next Friday to try and get the 3.5 trach in (might require outpatient surgery/sedation).
I left the appointment SO FRIGGIN’ ANGRY. The doctor just totally blew off my request, as he already had his mind up. He never looked at Hannah as the patient, he just saw “neuronopathic Gaucher’s disease” and that was it. It does not matter that she has a history of a unique presentation of the disease, it does not matter that she has had no lung issues whatsoever at this point, and it does not matter that her airway issues (vocal cord paresis and laryngomalacia) have significantly improved in the past year!
I felt like I was treated as a mom who knows nothing about my daughter’s medical condition. He would not even engage in a conversation about Hannah herself!
I got home from the appointment, and I called the ENT’s office to see if we could see him sooner than 9/3. He wasn’t available, but his partner was available to see Hannah to try and get the trach in tomorrow morning. We are going to keep the appointment on 9/3 with the ENT I wanted to use.
Dr. Roy, Hannah’s Houston ENT (and one of Hannah’s guardian angels), has a conference call set up with this new ENT on Monday to discuss Hannah’s case. Fortunately, Dr. Roy is also of the same mindset that I am that if Hannah does not need the trach now then take it out. You don’t trach a child because of a possible problem proactively if there are no issues even leading that way.
I also set up an new patient appointment with the other pediatric pulmonologist in town for next week. There are only two in this town, and I just do not feel comfortable going back to this doctor. I hope this doctor will, at the very least, give me the opportunity to discuss how I feel about the situation, even if he feels strongly that she needs to remained trach. I just hope that this doctor will be open-minded, that is the key. I hope, hope, hope that he is not like this other doctor.
I know that removing the trach may not be an option. But I want it to be because HANNAH, the person, needs the trach. Not because she has a diagnosis that may likely lead to an eventual trach so let’s not even consider it. Better safe than sorry is one thing but so is quality of life. If she needs to keep the trach in (and she may very well need to), then I want to be comfortable that it really is the right decision for her.
It is my right, as Hannah’s parent, to be involved in the decision to keep the trach or not. I am a smart enough mom, more educated on Gaucher’s disease than he is. He needs me and my experience and knowledge on Gaucher’s as much as I need him. He is the first doctor I have met since Hannah was born that has not treated our care of Hannah as a partnership.
Hopefully tomorrow will go better.
 When Hannah Ostrea was five months old, she was diagnosed with Gaucher’s disease, a genetic condition in which the body lacks the enzyme needed to break down a fatty waste product called glucocerebroside, leaving it toaccumulate in the body’s organs. The disease is painful, with the excess glucocerebroside impairing mobility and delaying growth. Hannah’s form of the disease, Neuronopathic Gaucher’s disease, also causes brain damage and eye movement disorders and makes swallowing difficult. Neuronopathic Gaucher’s affects less than 1 in 100,000 live births and the life expectancy of a sufferer is between two and 20 years — Hannah is now two. But because the medical community won’t dedicate time or money to an illness that affects so few, there is no cure on the horizon. “Unless you have a celebrity who has a personal interest in your disease or you have a ‘popular’ rare disease … there are no big foundations, large fundraisers, or even any interest in assistance,” says Hannah’s mother Carrie. “It’s so hard knowing that there is so little research out there for my daughter, and that because of this, we will likely lose her sooner rather than later.”
When Hannah Ostrea was five months old, she was diagnosed with Gaucher’s disease, a genetic condition in which the body lacks the enzyme needed to break down a fatty waste product called glucocerebroside, leaving it toaccumulate in the body’s organs. The disease is painful, with the excess glucocerebroside impairing mobility and delaying growth. Hannah’s form of the disease, Neuronopathic Gaucher’s disease, also causes brain damage and eye movement disorders and makes swallowing difficult. Neuronopathic Gaucher’s affects less than 1 in 100,000 live births and the life expectancy of a sufferer is between two and 20 years — Hannah is now two. But because the medical community won’t dedicate time or money to an illness that affects so few, there is no cure on the horizon. “Unless you have a celebrity who has a personal interest in your disease or you have a ‘popular’ rare disease … there are no big foundations, large fundraisers, or even any interest in assistance,” says Hannah’s mother Carrie. “It’s so hard knowing that there is so little research out there for my daughter, and that because of this, we will likely lose her sooner rather than later.”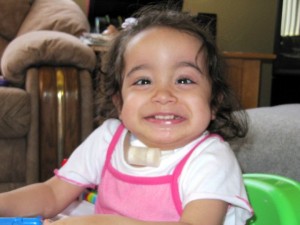




Latest Comments