This is a guest post from Tina M. from Kansas City, Missouri. She is the mom of Ethan, 23 months old, recently diagnosed with Gaucher’s Type 2.
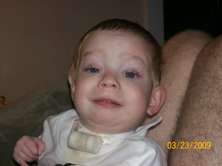 When we found out that we were having a little boy, we were ecstatic. The pregnancy was going great. We had no complications until we hit the seven month mark. Then the complications started, and haven’t ended yet. Ethan James McKown was born at 33 weeks. He was 4lbs 2oz and 19inches long. He was a little guy, but we knew right away he was a fighter. He did well in the NICU for 3 weeks and we finally got to take him home on the forth of July 2007.
When we found out that we were having a little boy, we were ecstatic. The pregnancy was going great. We had no complications until we hit the seven month mark. Then the complications started, and haven’t ended yet. Ethan James McKown was born at 33 weeks. He was 4lbs 2oz and 19inches long. He was a little guy, but we knew right away he was a fighter. He did well in the NICU for 3 weeks and we finally got to take him home on the forth of July 2007.
He always had large stomach but all the doctors in the NICU just simply said “he just has a large belly” and left it at that. We thought it was peculiar but we were so stressed with everything going on in the NICU that we didn’t think much of it at the time. Eventually he would grow out of it, right? We were wrong.
He went through a period where everything seemed to be getting back to normal. He started to get bronchiolitis/ bronchitis with severe double ear infections. We were fighting off every little cold and sniffle he would get. There was one night that we thought we were going to lose him. We knew he had a cold and we had taken him to his pediatrician and he gave us some cold medicine and said to keep and eye on him.
A couple of nights later we put him to bed and notice that he just wasn’t breathing right. We picked him up and tried to get him to respond to us or “liven” up a bit. He just looked at us exhausted, working very hard to breathe. When we couldn’t get him to keep his eyes open or breathe normally we decided we better take him to the ER. We went to the local hospital and it was a nightmare! They are not equipped to deal with a child that fragile and that little.
He was still very petite. Every nurse and every doctor in the ER were in that room. They did chest X-ray’s and everything else and finally made us leave the room because they had to put a breathing tube in. We were torn apart. Even the security guard who escorted us to the waiting room had tears in his eyes. We thought we were going to lose him. We called both of our parents at 2am and told them what was going on and sat and waited. The longest thirty minutes of our lives past by and we were finally allowed back to the room. He looked so helpless and completely drained of everything. The hospital had called for a transport to the area children’s hospital because they didn’t have the equipment to handle Ethan.
 The children’s hospital was about a forty-five minute drive away. We got to the children’s hospital and were immediate reassured everything was going to be alright. We were in very good hands then. They admitted him to a room and he had a bad case of bronchitis and the flu on top of it. His poor little body couldn’t keep up but he sure was fighting hard! We were there for about a week and were released to go home.
The children’s hospital was about a forty-five minute drive away. We got to the children’s hospital and were immediate reassured everything was going to be alright. We were in very good hands then. They admitted him to a room and he had a bad case of bronchitis and the flu on top of it. His poor little body couldn’t keep up but he sure was fighting hard! We were there for about a week and were released to go home.
Over the next 6 months or so we were in and out of the hospital at least once a month with respiratory issues, lack of weight gain, and various other issues.
Finally in April 2008 they admitted Ethan for failure to thrive and said that he wasn’t leaving until they found out what was wrong. They ran hundreds of tests in the week we were there. They first thought he had Cystic Fibrosis, but that test was negative. They drew more blood and finally told us we could go home because they would have to wait on results from some of the tests.
A week or two after we went home, we received a call stated plainly that we had an appointment in genetics the following week. That was it. No explanation, no reasoning, nothing.
May 5, 2008 two days after my husband’s 25th birthday our lives change forever. We met with Ethan’s genetics doctor and counselor and learned that he had Gaucher Disease. We had never heard of it and had no idea what we were up against. I have never felt so helpless or heartbroken in my life. They weren’t sure which type he had, but since he presented symptoms so early and already had neurological side effects, they were leaning towards type II but were hoping for Type III.
The next week he went into surgery to get a port placed so he could receive enzyme replacement therapy. We had quite the scare when he had trouble breathing after the sedation. About three weeks later, we received the results from his Type testing. While we were in the hospital with pneumonia, we found out that he had a homozygous L444P mutation. He had type III. We were so happy we cried that day. There was a chance for him. He would at least get treatment and hopefully live a healthy happy live. He was doing well with his treatments and everything was starting to get on track. He still wasn’t gaining weight, but his levels were good. Everything seemed to be looking up for us.
 I went to visit my brother in Topeka, KS which is about an hour away. Ethan would have breath holding spells, but none were as bad as that night. He went into a fit while grandma was feeding him. I took him from her and he stopped breathing. I immediately started CPR and tried to get him back. My brother called an ambulance but I luckily got him breathing again before they arrived. That was the longest three and half minutes of my life!
I went to visit my brother in Topeka, KS which is about an hour away. Ethan would have breath holding spells, but none were as bad as that night. He went into a fit while grandma was feeding him. I took him from her and he stopped breathing. I immediately started CPR and tried to get him back. My brother called an ambulance but I luckily got him breathing again before they arrived. That was the longest three and half minutes of my life!
After this episode, they scheduled a sleep study and realized that it was very dangerous for him to sleep. He would wake up about twenty times an hour because he would stop breathing. He was only getting two minutes of REM sleep a night. It was no wonder he wasn’t gaining weight. He was burning calories even when he was trying to sleep.
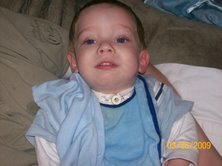
After seeing the results, the ENT clinic said that it was probably a good idea to have a tracheostomy tube put in. We were completely caught off guard with this. We didn’t know what to say but we had no choice. The risk of our son dying in his sleep was too high; we had to do the surgery. The scheduled it for the following day. They also did a surgery on his eyes to fix his strabismus.
When we saw him in the ICU after the surgery, I wanted to scoop him up in my arms and just go home. All we knew was our son was laying there with a tube in his throat to breathe through and blood filled tears. It was the most heart wrenching sight. He looked at us so confused. He couldn’t figure out why he couldn’t call out to us. He was trying to talk but no sound was coming out. His eyes would fill with tears which just made it worse. It is so hard to know that we won’t be able to hear his laugh again. We miss that more than anything.
He spent five days in the ICU and then another week on a floor before we were trained enough on how to take care of him.
A week before Christmas 2008, we went home and turned his nursery into a hospital room. We have oxygen sensors, liquid oxygen tanks, suction machine, CPR equipment, humidification machine. The list goes on. He started sleeping better and finally began to put on some weight, but not much.
In March of 2009 we had a gastrostomy tube placed and a nissen fundoplication because his acid reflux was so bad. He started to consistently gain weight and was doing better.
In April of 2009, they decided to send our blood off for more genetic testing because he was not responding to the treatments like a typical Type III patient would. We received the results a few weeks later. The results were not good. Ethan in fact has one copy of L444P gene and one copy of L444P, A456P, and V460V:1497G>C gene. His genetics doctors have never seen this variant of the disease before.
Ethan has Type II Gaucher Disease. Our world has changed forever. We just found out that our son probably will not live to see his third birthday.
We will be forced to stop his enzyme replacement therapy and he will slowly begin to fade away from us. We cannot understand why they will not allow us to continue the treatment when it seems to be doing him good. Why must they give up on our son?
 Can you believe it has been three months since
Can you believe it has been three months since 
Latest Comments